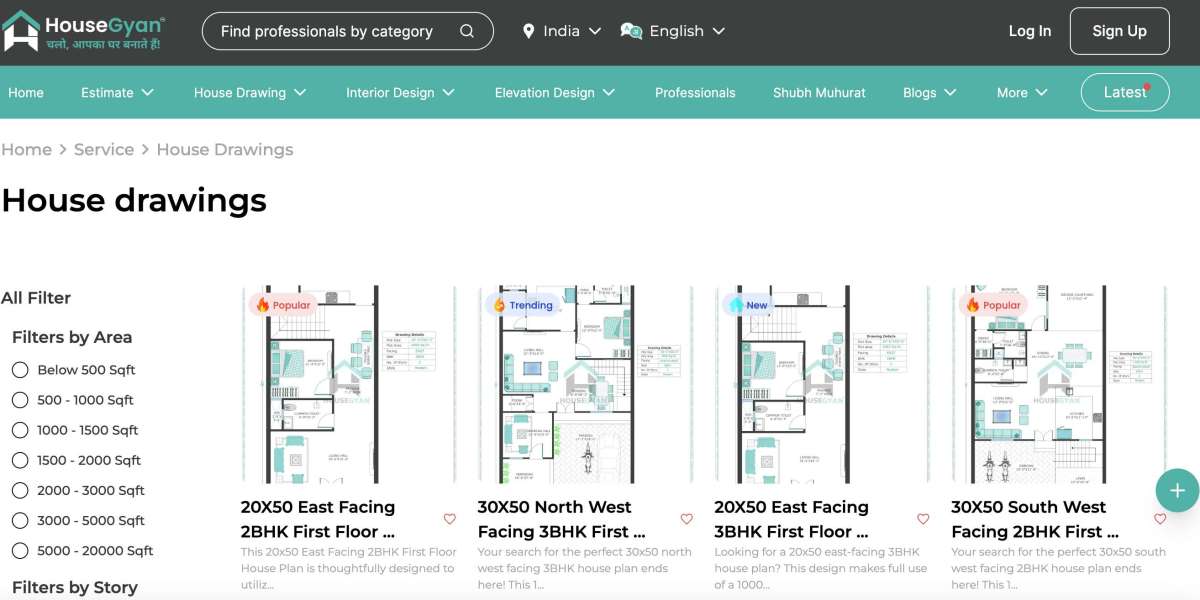
Medical billing services are being used by healthcare providers more and more to handle intricate billing procedures, enhance claim accuracy, and stay in line with industry standards. It becomes crucial for enterprises to make sure the billing partner adheres to stringent compliance standards when they choose to outsource medical billing services. Compliance guarantees proper reimbursement from insurance payers, lowers legal risks, and safeguards patient information.
HIPAA (Health Insurance Portability and Accountability Act) compliance is one of the most crucial requirements for medical billing businesses. Billing providers must adhere to stringent privacy and security protocols and safeguard patient health information in accordance with HIPAA laws. When conducting operations like charge entry in medical billing services or submitting claims, outsourced billing teams are required to employ secure systems, encrypted communication routes, and regulated access to patient data. Healthcare providers can avoid fines and preserve patient privacy by adhering to HIPAA regulations.
Adhering to appropriate coding standards, such as ICD-10, CPT, and HCPCS codes, is another crucial aspect of compliance. Correct documentation and billing of healthcare services in accordance with payer rules are guaranteed by accurate coding. Billing professionals must remain current on payer regulations and frequent code changes when working with hospital medical billing services. Denials of claims, late payments, or noncompliance might result from mistakes in coding or documentation.
Federal and payer-specific billing laws must also be followed by outsourced billing companies. Providers must adhere to stringent billing regulations set forth by healthcare payers, such as Medicare, Medicaid, and private insurance companies. Reliable billing partners use cutting-edge medical billing services software to automate compliance checks, identify coding issues, and guarantee that claims fulfill payer standards prior to submission. These solutions increase first-pass claim acceptance rates and decrease billing errors.
Another crucial duty for billing organizations is adherence to audit and documentation standards. Outsourced billing partners are required to keep proper records of patient treatments, billing transactions, and claim histories since healthcare providers may be audited by government authorities or insurance companies. In addition to promoting transparency, appropriate documentation guarantees that the billing procedure is compliant with legal requirements.
Medical billing services with efficient denial handling are also crucial to compliance. In accordance with payer requirements, billing providers must examine rejected claims, fix any mistakes, and submit them again. Billing teams can find persistent compliance problems and stop future claim rejections by keeping an organized denial management procedure.
When assessing the cost of medical billing services, healthcare providers also need to take financial transparency into account. Billing firms are required to provide a comprehensive description of their service agreements, pricing methods, and reporting procedures. Providers can better assess their revenue cycle performance and make sure there are no unapproved or hidden costs by using transparent billing procedures.
Outsourcing medical billing services has advantages beyond increased administrative effectiveness. Billing partners that prioritize compliance enhance financial performance, lower the chance of regulatory infractions, and increase claim accuracy. Outsourcing enables many healthcare firms to concentrate on patient care while skilled billing specialists handle intricate regulatory needs.
In the end, provider practices' medical billing services need to adhere to stringent healthcare rules, keep accurate records, and make use of safe technological platforms. In an increasingly complicated healthcare environment, healthcare providers can enhance revenue cycle management, reduce claim denials, and maintain complete regulatory compliance by collaborating with knowledgeable and compliant billing specialists.