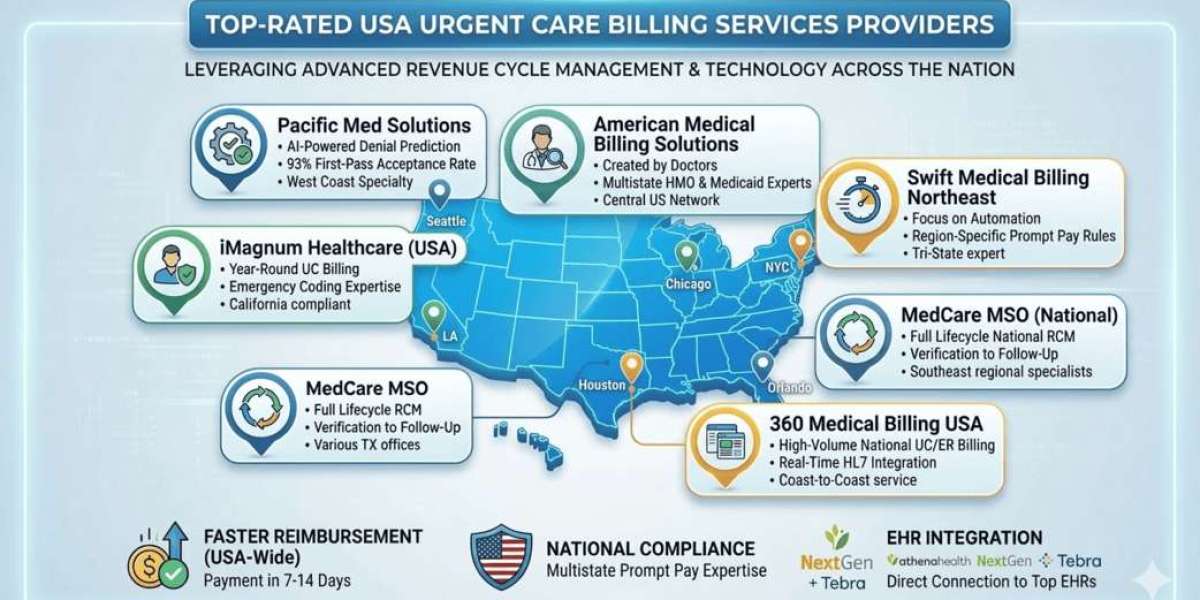
Urgent care centers play a vital role in the U.S. healthcare system by providing immediate treatment for non-life-threatening conditions. These facilities manage a high patient volume every day, which makes accurate documentation, coding, and billing essential for maintaining financial stability. Coding and billing for urgent care requires a deep understanding of payer rules, CPT and ICD-10 codes, compliance standards, and efficient revenue cycle workflows.
Unlike traditional physician practices, urgent care facilities treat a wide range of acute conditions and perform various procedures in a single visit. This diversity creates unique challenges in medical billing for urgent care, including correct code selection, modifier usage, and claim submission timelines.
Understanding how urgent care billing works can help providers reduce denials, improve reimbursement, and maintain regulatory compliance.
Key aspects of urgent care coding and billing include:
Accurate documentation of patient visits ensures correct CPT and ICD-10 code selection.
Proper modifier usage helps differentiate procedures performed during the same visit.
Timely claim submission improves reimbursement cycles and reduces payment delays.
Eligibility verification prevents claim rejections due to insurance coverage issues.
Compliance with payer policies ensures accurate billing for urgent care services.
A well-structured urgent care billing workflow supports operational efficiency and helps healthcare providers focus more on patient care rather than administrative challenges.
Understanding Coding and Billing for Urgent Care
Coding and billing for urgent care involves translating clinical documentation into standardized medical codes and submitting claims to insurance payers for reimbursement. This process includes CPT codes for procedures, ICD-10 codes for diagnoses, and HCPCS codes for specific services or supplies.
Urgent care facilities commonly treat conditions such as minor injuries, infections, respiratory illnesses, and diagnostic testing. Each service performed during a visit must be documented correctly to support the claim submitted to insurance carriers.
Medical coding specialists review physician documentation and assign appropriate codes. Once coding is completed, the billing team prepares and submits claims, tracks payments, manages denials, and ensures compliance with payer regulations.
Due to the complexity of services provided in urgent care centers, many healthcare providers rely on professional urgent care billing and coding services to maintain accuracy and efficiency.
Common Services Billed in Urgent Care Centers
Urgent care clinics provide a broad spectrum of medical services that must be coded and billed correctly. The most common services include:
Evaluation and management visits are the foundation of urgent care billing. Providers document the patient’s symptoms, examination findings, and medical decision-making to determine the correct E/M code.
Diagnostic services such as X-rays, laboratory testing, and rapid screenings are frequently performed during urgent care visits. Each diagnostic service requires proper coding and supporting documentation.
Minor procedures including wound repair, splinting, incision and drainage, and foreign body removal are often performed in urgent care settings. These procedures must be coded separately from evaluation services when appropriate.
Vaccinations and injections are another common service billed in urgent care centers. These services require both administration codes and vaccine product codes.
Accurate coding of these services plays a major role in efficient urgent care medical billing and helps ensure providers receive proper reimbursement.
Challenges in Urgent Care Billing and Coding
Urgent care facilities often face several billing challenges due to the fast-paced nature of their operations. High patient volumes and varied treatment types increase the risk of documentation errors and coding mistakes.
One common challenge is improper code selection. Without accurate coding, claims may be rejected or underpaid by insurance providers. Another issue involves incorrect modifier usage, which can result in claim denials.
Insurance verification errors can also affect billing outcomes. When patient coverage is not verified properly, claims may be rejected due to eligibility issues.
Additionally, urgent care centers must keep up with frequent updates to medical coding guidelines and payer policies. These changes require continuous training and monitoring to maintain compliance.
For these reasons, many healthcare organizations choose urgent care billing outsourcing solutions to manage their billing operations effectively.
The Role of Professional Urgent Care Billing Services
Professional urgent care billing services help healthcare providers streamline the entire revenue cycle process. These services typically include medical coding, claim submission, denial management, payment posting, and compliance monitoring.
An experienced urgent care billing services company understands the specific requirements of urgent care centers and works to minimize claim errors. Their teams stay updated on regulatory changes and payer guidelines, ensuring accurate billing for urgent care services.
Specialized billing teams also track claims and identify potential revenue leaks. By analyzing billing trends and denial patterns, they help providers optimize their financial performance.
Healthcare organizations looking for reliable billing support often partner with urgent care billing companies that focus exclusively on urgent care operations.
Regional Urgent Care Billing Support in the United States
Urgent care facilities across different states may face varying insurance regulations and payer requirements. As a result, specialized regional billing services have become increasingly popular.
For example, providers seeking billing for urgent care services Florida often work with experts familiar with local payer guidelines and reimbursement policies. A florida urgent care billing services provider can help clinics navigate state-specific regulations and improve claim acceptance rates.
Similarly, clinics operating in Texas often rely on texas urgent care medical billing services to manage their claims efficiently. A texas urgent care billing services provider understands regional insurance networks and can streamline the billing workflow for urgent care centers in the state.
These specialized services ensure compliance while improving financial outcomes for urgent care providers.
Benefits of Outsourced Urgent Care Medical Billing
Outsourcing billing operations has become a strategic decision for many healthcare providers. Outsourced urgent care medical billing allows clinics to focus on patient care while experts handle the complex billing processes.
One of the major benefits is improved claim accuracy. Experienced billing professionals understand coding guidelines and payer rules, which reduces errors and denials.
Another advantage is faster reimbursement. Efficient claim submission and follow-up processes help accelerate the payment cycle and improve cash flow.
Outsourcing also reduces administrative workload for internal staff. Instead of managing billing tasks, clinic teams can focus on patient engagement and operational efficiency.
Healthcare providers often partner with an urgent care billing agency or an urgent care billing provider that offers end-to-end billing support and revenue optimization.
Key Components of an Effective Urgent Care Billing Process
A successful urgent care billing system involves multiple stages within the revenue cycle.
Patient registration and insurance verification ensure that accurate information is collected before the visit begins. This step reduces the risk of claim rejection.
Medical coding converts clinical documentation into standardized codes used by insurance payers. Proper coding ensures accurate billing for services rendered.
Claim submission involves sending coded claims electronically to insurance companies. Efficient submission reduces delays in processing.
Payment posting records payments received from insurers and patients. This step helps track revenue and identify outstanding balances.
Denial management involves reviewing rejected claims, correcting errors, and resubmitting them for reimbursement. Effective denial management is crucial for maximizing revenue.
When managed properly, these components create efficient urgent care billing solutions that support the financial health of healthcare organizations.
Technology and Automation in Urgent Care Billing
Modern urgent care billing services increasingly rely on advanced technology to streamline billing workflows. Electronic health records and practice management systems integrate clinical documentation with billing processes.
Automation tools help reduce manual errors and speed up claim processing. For example, automated eligibility verification checks insurance coverage before patient visits.
Billing analytics platforms allow providers to monitor key performance indicators such as claim acceptance rates, denial percentages, and average reimbursement times.
By adopting advanced urgent care billing solutions, healthcare providers can improve accuracy, transparency, and financial performance.
Choosing the Right Urgent Care Billing Partner
Selecting the right urgent care billing services provider is essential for maintaining efficient revenue cycle operations. Healthcare providers should consider several factors when evaluating billing partners.
Industry experience is critical. A company specializing in urgent care center medical billing services understands the complexities of urgent care coding and payer requirements.
Technology capabilities also play an important role. Advanced billing platforms and reporting tools help improve transparency and performance tracking.
Compliance expertise ensures that billing operations follow current healthcare regulations and payer guidelines.
Finally, scalability is important for growing healthcare organizations. A reliable urgent care billing provider can adapt to increasing patient volumes and evolving operational needs.
How Professional Billing Services Improve Urgent Care Revenue
A structured billing approach significantly improves financial outcomes for urgent care facilities. With accurate documentation, proper coding, and timely claim submission, providers can reduce denials and increase reimbursements.
Experienced urgent care billing companies also conduct regular audits to identify coding errors and compliance risks. These audits help maintain accurate billing practices and prevent revenue loss.
Revenue optimization strategies such as denial analysis, claim tracking, and payment reconciliation further enhance the financial performance of urgent care clinics.
When healthcare organizations adopt professional urgent care billing and coding services, they gain access to specialized expertise that improves overall revenue cycle management.
Conclusion
Coding and billing for urgent care is a complex but essential component of healthcare operations in the United States. With high patient volumes and diverse treatment services, urgent care centers must maintain accurate documentation, proper coding, and efficient billing processes to ensure financial sustainability.
Professional urgent care billing services help providers navigate the challenges of insurance claims, coding guidelines, and regulatory compliance. Whether clinics choose outsourced urgent care medical billing or work with a specialized urgent care billing agency, the right billing strategy can significantly improve reimbursement outcomes.
Organizations such as 247 Medical Billing Services support healthcare providers with comprehensive solutions including medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services. These integrated services help urgent care centers streamline their operations and focus on delivering quality patient care while maintaining strong financial performance.
Frequently Asked Questions
What is coding and billing for urgent care?
Coding and billing for urgent care refers to the process of converting patient visit documentation into standardized medical codes and submitting insurance claims for reimbursement of services provided at urgent care centers.
Why is accurate urgent care medical billing important?
Accurate urgent care medical billing ensures proper reimbursement, reduces claim denials, maintains compliance with insurance regulations, and improves overall financial stability for healthcare providers.
What services are commonly billed in urgent care centers?
Urgent care centers typically bill for evaluation and management visits, diagnostic tests, minor procedures, vaccinations, and laboratory services performed during patient visits.
Why do urgent care centers outsource billing services?
Many providers choose urgent care billing outsourcing to improve claim accuracy, reduce administrative workload, accelerate reimbursements, and ensure compliance with evolving healthcare regulations.
How do urgent care billing companies improve revenue cycle management?
Urgent care billing companies handle coding, claim submission, denial management, payment posting, and compliance monitoring, helping healthcare providers optimize revenue and reduce financial risks.
What should providers look for in an urgent care billing services company?
Healthcare providers should look for industry experience, advanced technology solutions, compliance expertise, transparent reporting, and scalable services when selecting an urgent care billing services company.