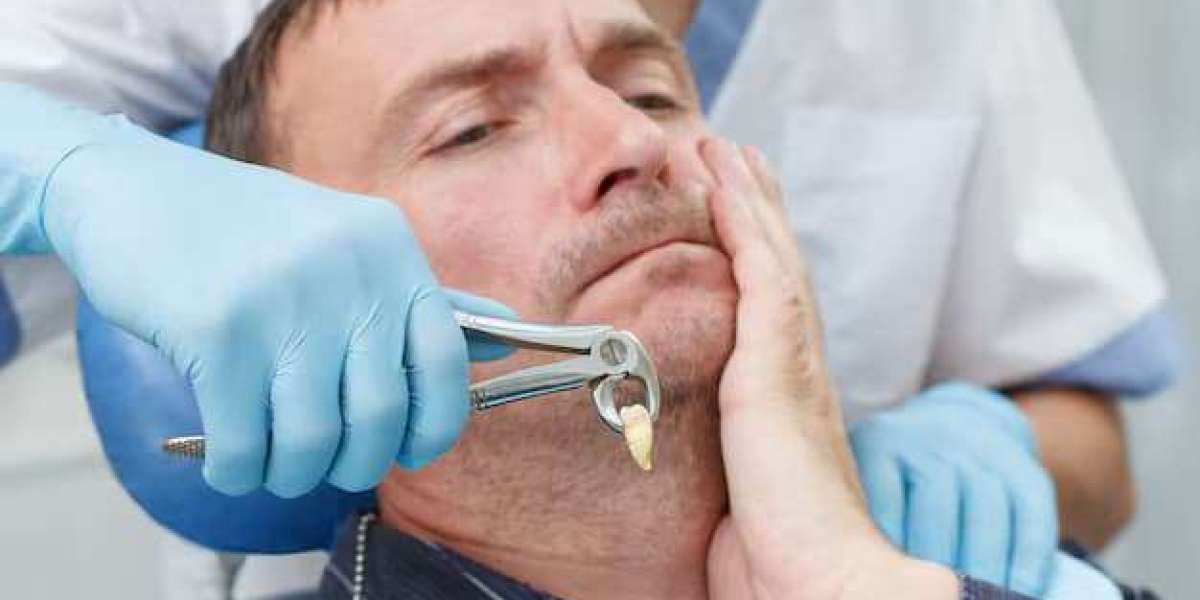
Impacted teeth are a common dental concern that can lead to discomfort, infection, and complications if left untreated. When a tooth becomes trapped beneath the gums or fails to emerge properly, dental professionals may recommend extraction to protect overall oral health. Many individuals facing this condition seek professional guidance for oxnard tooth extraction to address impacted teeth safely and effectively. Understanding why teeth become impacted, how extraction works, and what to expect during recovery can help patients feel more confident and prepared when considering treatment.
Understanding Impacted Teeth
What Are Impacted Teeth
Impacted teeth occur when a tooth does not have enough space to grow or emerge normally through the gums. This often happens when nearby teeth block its path or when the jaw does not have adequate room to accommodate the tooth. The tooth may remain partially or completely trapped beneath the gum tissue or bone. Impacted teeth can develop gradually and may not cause immediate symptoms, but over time they can lead to pain, swelling, or infection that requires professional treatment.
Common Teeth That Become Impacted
While any tooth can become impacted, wisdom teeth are the most commonly affected. These are the last molars that usually appear during late teenage years or early adulthood. Because they erupt later, there may not be enough space left in the mouth for them to grow properly. Other teeth that sometimes become impacted include canines and premolars. Dentists closely monitor tooth development and alignment to determine whether extraction is necessary to prevent complications.
Causes of Tooth Impaction
Lack of Space in the Jaw
One of the primary reasons teeth become impacted is insufficient space in the jaw. When the jawbone does not have enough room for all the teeth to emerge properly, some teeth may become trapped beneath the gums or grow at unusual angles. This lack of space can cause pressure on surrounding teeth and may result in discomfort, crowding, or shifting of the dental alignment. Early evaluation can help identify these concerns before they worsen.
Abnormal Tooth Position
Sometimes a tooth becomes impacted because it grows at an unusual angle. Instead of moving upward into its proper position, the tooth may tilt sideways, backward, or forward within the jawbone. This irregular positioning prevents the tooth from emerging correctly and may cause it to press against neighboring teeth. Over time, the abnormal pressure can damage adjacent teeth or create areas where bacteria accumulate, increasing the risk of infection and gum disease.
Delayed Tooth Eruption
In certain cases, teeth simply fail to erupt on schedule. Delayed eruption may occur because of genetic factors, developmental issues, or problems with the surrounding bone structure. When a tooth remains trapped beneath the gums for an extended period, it may eventually become impacted. Dental professionals often monitor tooth development with regular examinations and imaging to detect any delays and recommend treatment if necessary.
Symptoms of Impacted Teeth
Pain and Discomfort
Pain is one of the most common symptoms associated with impacted teeth. The pressure created by a tooth trying to emerge in a limited space can cause soreness in the jaw or gums. This discomfort may be constant or may occur only when chewing or biting. Some individuals experience intermittent pain that gradually becomes more noticeable as the tooth continues to push against surrounding tissues.
Swelling and Gum Irritation
Swelling around the affected area is another common sign of an impacted tooth. The gum tissue covering the trapped tooth may become inflamed, red, or tender. In some cases, food particles and bacteria can collect around the partially erupted tooth, leading to irritation or infection. Persistent swelling should be evaluated by a dental professional to prevent more serious complications from developing.
Difficulty Opening the Mouth
Impacted teeth can sometimes cause stiffness in the jaw, making it difficult to open the mouth fully. This condition occurs when inflammation spreads to nearby muscles and tissues. Individuals may notice discomfort while speaking, chewing, or yawning. If jaw stiffness persists, professional evaluation is important to determine whether an impacted tooth is contributing to the problem.
Why Tooth Extraction May Be Necessary
Preventing Infection and Decay
When a tooth is impacted, it can create small spaces where bacteria accumulate. These areas are difficult to clean effectively with regular brushing and flossing. Over time, trapped bacteria may lead to tooth decay or infections in the surrounding gum tissue. Removing the impacted tooth helps eliminate these problem areas and protects the health of neighboring teeth.
Protecting Nearby Teeth
An impacted tooth can place pressure on adjacent teeth, potentially causing damage or misalignment. As the impacted tooth pushes against nearby structures, it may weaken the roots of neighboring teeth or shift them out of their natural positions. Extraction can relieve this pressure and help maintain proper alignment within the mouth, preventing long term complications.
Preventing Cysts and Other Complications
In some cases, impacted teeth can lead to the development of cysts or other growths within the jawbone. These fluid filled sacs may damage surrounding bone and tissues if not treated promptly. Although this complication is not extremely common, it is one reason dentists often recommend removing impacted teeth before problems escalate. Early intervention reduces the risk of serious oral health issues.
The Tooth Extraction Process
Initial Examination and Diagnosis
Before recommending extraction, dental professionals perform a thorough examination to assess the position and condition of the impacted tooth. Imaging techniques such as dental X rays help reveal the exact location of the tooth within the jaw. This information allows the dentist to determine the best approach for removing the tooth safely while minimizing discomfort and protecting nearby structures.
Preparing for the Procedure
Preparation for extraction typically involves discussing the procedure and reviewing the patient's medical history. Local anesthesia is commonly used to numb the treatment area and ensure comfort during the procedure. In some cases, additional sedation may be offered depending on the complexity of the extraction and the patient's level of anxiety. Proper preparation helps ensure that the procedure is performed efficiently and safely.
Removing the Impacted Tooth
During the extraction process, the dentist carefully accesses the impacted tooth through the gum tissue. In some situations, a small portion of bone surrounding the tooth may need to be removed to create enough space for extraction. The tooth may be removed in sections to make the process smoother and reduce stress on the surrounding tissues. Once the tooth is removed, the area is cleaned and prepared for healing.
Recovery After Tooth Extraction
Managing Discomfort
After the procedure, mild discomfort and swelling are normal as the body begins to heal. Dental professionals typically recommend rest and the use of cold compresses to reduce swelling during the first day. Over the counter pain relievers may also be suggested to help manage any discomfort. Most patients notice gradual improvement within a few days as the extraction site begins to heal.
Following Aftercare Instructions
Proper aftercare is essential for a smooth recovery. Patients are usually advised to avoid vigorous rinsing, smoking, or drinking through a straw for the first few days. These actions can interfere with the healing process and may lead to complications such as dry socket. Gentle oral hygiene and following the dentist's instructions help ensure that the extraction site heals properly.
Monitoring the Healing Process
Healing after tooth extraction typically progresses over several days to a few weeks. During this time, the gum tissue gradually closes over the extraction site and the underlying bone begins to regenerate. Patients should attend any recommended follow up visits to ensure that the area is healing correctly. If unusual pain, swelling, or bleeding occurs, contacting a dental professional promptly is important.
Preventing Future Dental Complications
Regular Dental Checkups
Routine dental visits play a significant role in preventing complications related to impacted teeth. During these appointments, dentists evaluate the development and alignment of teeth, allowing them to identify potential issues early. Early detection provides the opportunity to address problems before they lead to discomfort or more complex treatments.
Maintaining Good Oral Hygiene
Proper oral hygiene is essential for maintaining healthy teeth and gums. Brushing at least twice a day, flossing daily, and using recommended oral care products help prevent plaque buildup and infections. Keeping the mouth clean also supports faster healing after dental procedures and reduces the risk of future dental concerns.
Monitoring Wisdom Teeth Development
For many individuals, wisdom teeth are the most likely teeth to become impacted. Dentists often monitor their development during routine checkups and may recommend imaging to evaluate their position within the jaw. Early assessment helps determine whether these teeth have enough space to emerge properly or if preventive extraction may be beneficial.
Conclusion
Impacted teeth can cause a range of dental problems, from persistent discomfort to infections and damage to nearby teeth. Understanding the causes, symptoms, and treatment options allows individuals to make informed decisions about their oral health. Individuals seeking professional care and guidance can turn to puridentistry for safe and reliable tooth extraction, ensuring proper treatment and recovery. Tooth extraction is often recommended to prevent complications and maintain proper dental alignment. With professional care and proper aftercare, recovery can be smooth and successful.
Click here to learn more about comprehensive dental care in Oxnard.